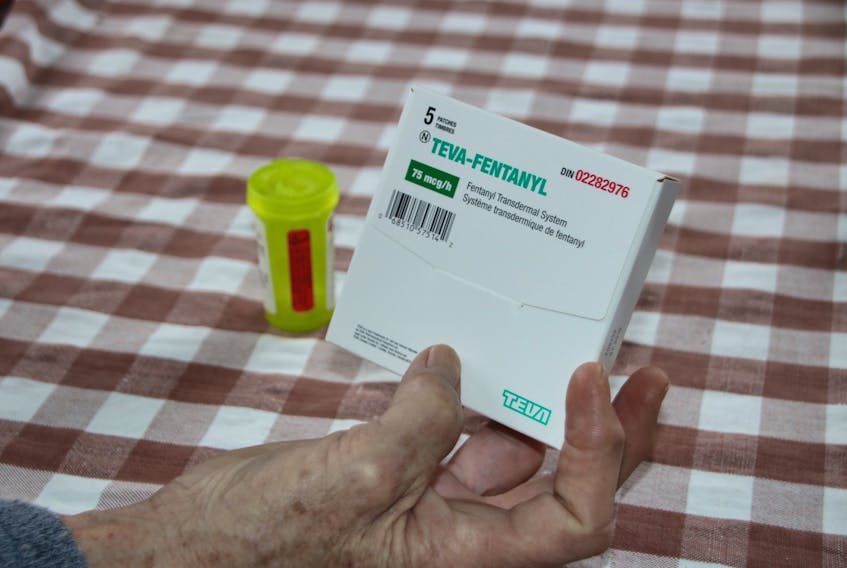
TRURO, N.S. — The pain. The growing agitation.
The excruciating symptoms of drug withdrawal are overtaking Carma.
The Truro woman is so tired and sore, most times it’s best she doesn’t move. The cramps come in waves, and are sometimes so relentless, she has trouble breathing.
But in a world where opioid addiction is rampant, this is a very different story.
Carma’s going through withdrawal because she no longer has a family doctor to prescribe vital medication for her pain or to help her come off those meds safely.
These legally acquired opioids had been a blessing. Now comes the curse.
“The pain is getting worse and the spasms are ridiculous,” said Carma (not her real name). “I feel I’m having a heart attack at times; my blood pressure is so high.
“My joints and muscles are so sore I can hardly move by neck and my stomach hurts so much it feels like it’s touching my backbone. I can feel the nerve endings; even under my fingernails I can feel the nerves and I just want to scratch.
“I want to crawl out of my body because there’s nothing I can do to stop the pain."
“I want to crawl out of my body because there’s nothing I can do to stop the pain. My energy’s been zapped, I get annoyed with the world and I feel useless.”
Because she had injuries from sporting accidents, and has arthritis, her doctor prescribed pain medication for her. She tried several options before being prescribed Fentanyl and hydromorphone 10 years ago.
“They didn’t cause any issues, and they helped me get my life back,” she said.
“When I heard my family doctor was closing his practice, I put my name on the list for a new doctor, with no luck. On my last visit to my family doctor, he gave me enough medication to last a while and a slip of paper with information on withdrawal.
Carma called several doctors’ offices and clinics, from Truro to Halifax, only to be told to put her name on “the list.” It was the same message from the College of Physicians and Surgeons of Nova Scotia, and Doctors Nova Scotia. The pain clinic told her she needed a referral from a family doctor. The opioid clinic told her to get an overdose kit from her pharmacy.
“I had an interview with a doctor in Waverley, and when he heard I am on opioids he stood up, shook my hand, said he doesn’t deal with them and left the room – with me begging for help,” she said. “I had an interview with a doctor in Dartmouth, same thing. I’m not asking them for more opioids, just help coming off them.”
A psychologist suggested addiction services. They told her to put her name on the list and go to a walk-in clinic. Both local clinics told her to go to emergency.
"I’m not asking them for more opioids, just help coming off them.”
“I called emergency and the woman I spoke with told me to come over, there was a psychiatrist on duty. My husband and I went over and when we were called into the family interview room the doctor yelled, saying they don’t prescribe those drugs there, and I should find a family doctor. I told him I had called and was told to come over, but when I couldn’t tell him the name of the person I had talked to, he accused me of lying. When I asked what his name was, he yelled again, asking if I was threatening him. We had to ask him, more than once, to calm down.
“I was going through withdrawal, experiencing depression because of it, and then I was demeaned by the doctor.”
The physician eventually relented and gave her three hydromorphone patches and four Fentanyl tablets. He also told her not to come back for more.
In an effort to wean herself from the medication, Carma had her Fentanyl dosage reduced and has cut the patches into smaller pieces. Now they’re almost gone.
“I’ve been put in this vulnerable situation and everywhere I’ve gone for help they’ve passed me off to someone else,” she said. “I’m devastated at the lack of compassion and help, and I can’t be the only one going through this. I’m very frustrated and feeling at wit’s end.”
"Patients like this end up being orphaned." - Kevin Chapman
Kevin Chapman, director of partnerships and finance with Doctors Nova Scotia, acknowledges people like Carma are not receiving the care they need, due to gaps in the system.
“It’s a sad occurrence,” he said. “We don’t have enough primary care providers, and patients like this end up being orphaned.”
He said it’s difficult for a physician to treat someone who is on opioids if they don’t know them well, but some will write prescriptions for short periods of time. There are concerns, when the doctor doesn’t know the patient, about whether medication is being used properly.
“Walk-in clinics are for episodic care and this is for continuity of care. Unfortunately, with the paucity of primary care providers now, there aren’t a lot of options other than emergency. I wish I had more helpful advice.
“This speaks to why we need primary care stability in Nova Scotia. Physician recruitment has to be a priority.”
Asked about patients facing dilemmas similar to Carma’s, the primary health team of the Nova Scotia Health Authority chose to respond by email, essentially reiterating their policy for acquiring a family doctor, and acknowledging this “can sometimes be a challenge.”
However, they also indicated, “The College of Physicians and Surgeons of Nova Scotia has professional standards for family doctors who are closing their practice, which indicates that a physician should make reasonable efforts to provide assistance for patients with complex care needs, including transfer and follow-up care.”
They also assured their commitment to “recruiting every day for health care professionals...”
RELATED